What is a care path?
A care path includes all the phases of your patient care
From the moment cancer diagnosis is confirmed, during the disclosure appointment, the doctor explains and provides the patient with a personal care plan (PCP) summarising the different treatment phases. It can also include referral for oncology supportive care. Each patient follows their own personal care path.
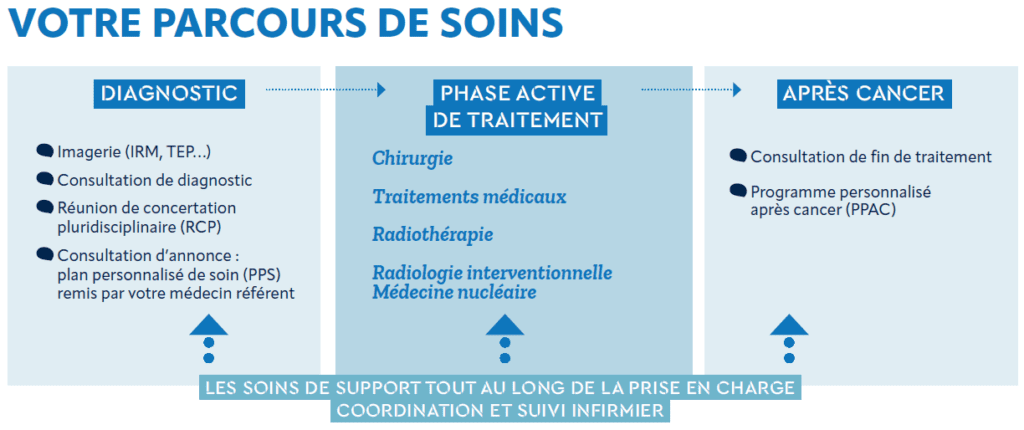
The care path relies on a multidisciplinary medical team and professionals from different fields, who act as an interface with the general practitioner and external specialised practitioners.
Those involved in your care path at the centre
Your consulting physician
This is the doctor who, at the Centre François Baclesse, coordinates all your diagnostic, therapeutic and follow-up phases. They work in close collaboration with all teams within the centre and with external healthcare professionals. They systematically inform your GP (with your consent) of each phase of your care path.
Your care path nurses
Accompanying nurses are specifically entrusted with ensuring your personal monitoring throughout your care path, via permanent links with your consulting physician and all other professionals involved in your care, both within and outside the centre, such as GPs, community and district nurses, dispensing chemists, etc.
Their role is to:
- Complete information provided by the consulting physician,
- Propose access to supportive care at the centre.
Care path nurse contact information
| THE CARE PATHS | Telephone hotline |
|---|---|
| BREAST CANCER / SARCOMAS / CANCER OF UNKNOWN PRIMARY SITE | +33(0)2 31 45 86 48 |
| UAT / CHEST / NEURO-ONCOLOGY | +33(0)2 31 45 40 71 |
| GYNAECOLOGIE / UROLOGY / DIGESTIVE SYSTEM | +33(0)2 31 45 86 74 |
Key elements in care safety
The Multidisciplinary Team Meeting (MDT)
The MDT meeting reunites doctors from different specialities likely to be involved in the patient’s care. The GP is systematically invited to attend. It is during MDT meetings that decisions on treatment are made, based on adapted strategic reflection. After the MDT meeting, a detailed report is drafted and sent to the patient’s GP. During a medical consultation, the discussion is repeated to the patient and a Personal Care Plan is provided.
At the Centre François Baclesse, several MDT meetings specific to different types of cancers treated at the centre are organised every week.
The Personal Care Plan (PCP)
Once the proposed treatment has been validated by the MDT, a Personal Care Plan is given to the patient by the consulting physician. This plan presents the different treatment phases and their chronology, hence offering an overview of the patient’s care path.
Care continuity: the hospital care – external care link
Each time a patient consults or is hospitalised at the centre, a specific medical letter is sent to his/her general practitioner. The consulting physician at the centre is generally informed.
If the situation requires so, a letter can also be sent to other healthcare professionals.
The personal Survivorship Care Plan
When treatment is complete, we then refer to the ‘post-cancer period’. Medical follow-up is organised. Social worker guidance, access to supportive care and referral to external healthcare providers can also be proposed. All of these elements are noted in a Survivorship Care Plan (SCP).
To best prepare this period, an appointment with the consulting physician and the care path nurses is systematically proposed to all patients.
