A CT scan is a radiological examination, more technically referred to as tomodensitometry or TDM. It is conducted in the radiology unit of the medical imaging department.
What is a CT scan?
This imaging technique uses an X-ray machine to create images of a part of your body (doses are the lowest possible and are limited to examined zones). The associated radiation is of no danger to you or your close circle.
The CT scan can enable your organs to be viewed, to look for potential lesions, be they benign or malignant. Hundreds of pictures of the inside your body are taken and can be viewed in cross-sections on a computer screen.
Most CT scans require for an iodine-based contrast agent to be injected. This renders certain parts of the body opaque, so they are easier to view.
What happens during the scan?
The injection of an iodine-based solution is frequent but not systematic; it depends on the organ to be analysed. If an injection is required, you will be given a prescription and will need to collect the product at your local dispensing chemist, and bring it with you on the day of your scan.
The injection is made into a vein in the arm, also for patients with an implanted port, for the iodine product is too thick to be administered via this port. When the product is injected, patients often feel a sensation of heat or have a strange taste in their mouths. Both the CT scan and the injection are painless.
The most frequently observed side effects are:
- An allergic reaction to the contrast agent, particularly if you already have a history of allergies. This unpredictable reaction is generally temporary and minor. It can be more serious and require treatment.
- Alteration in kidney function; this is why we ask you to have a blood test to assess your kidney function before the scan (measurement of creatinaemia and creatinine clearance), and to drink a lot of water before and after the scan.
What you need to tell the medical team
Special precautions are taken based on the information you provide when you make the appointment and before the scan.
If you are pregnant or potentially pregnant (late period), if your are diabetic or if you suffer from kidney disease (kidney failure), please remind the radiologist.
If you feel pain or an unpleasant sensation, let the medical or paramedical staff know and someone will stay by your side during the scan.
The day of the scan: get prepared
- You do not need to come to the scan with an empty stomach (unless in excpetional cases of which you will be informed beforehand).
- Do not smoke during the hours that precede the scan.
- Unless specified otherwise, you can drink normally and, if necessary, take your usual medication.
- When you arrive in the department, you will be asked to remove all jewellery and metallic objects you are wearing (piercing, bras, keys, etc.) and leave them in the changing cabin provided.
During the scan
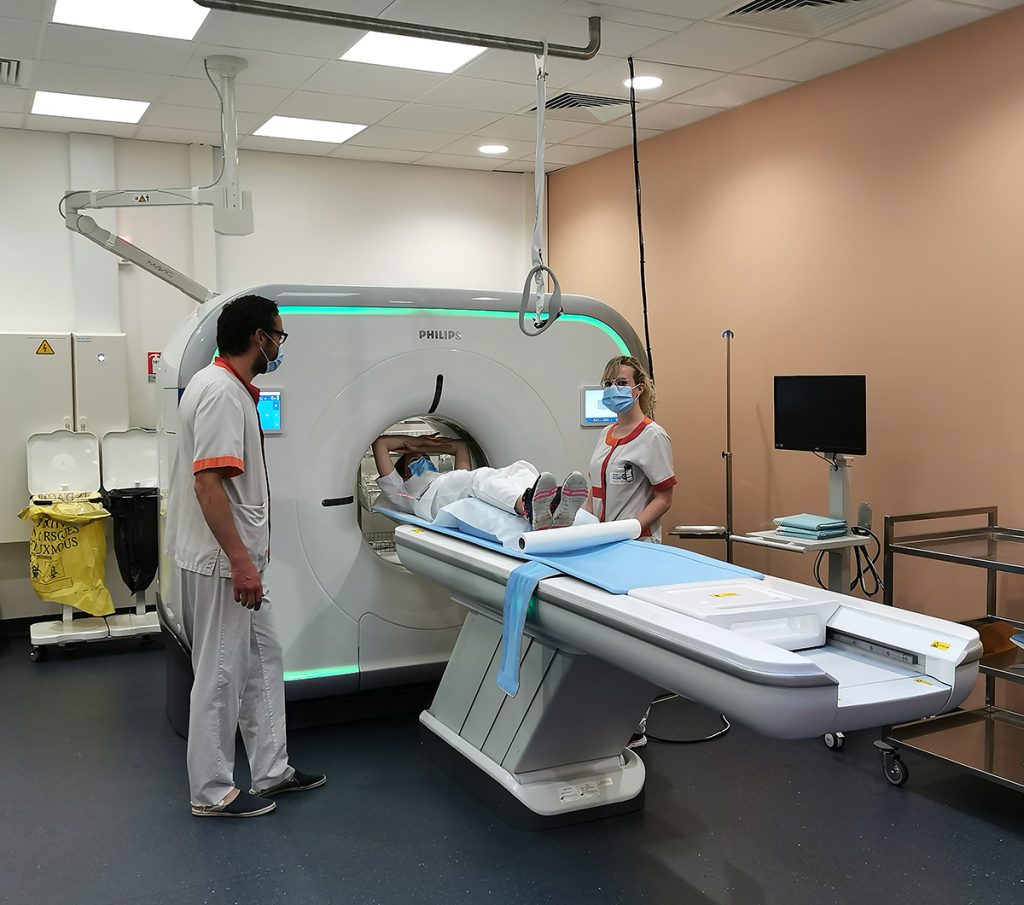
You lie on your back, most often with your arms behind your head or at the sides of your body, on an examination table which will slowly move inside a large ring. This is where the different images are taken.
You must try to stay as still as possible. The medical team stays in contact with you thanks to a microphone, and may ask you to hold your breath several times.
The scan takes around 10 to 15 minutes
NB: if you suffer from pain when lying down, and for your comfort, please take pain-relief medication 45 to 60 minutes before the scan. Tell the doctor who prescribed the scan.
What to do after the scan
In most cases, there are no side effects. There is no particular precaution to be taken! No change in your lifestyle will be necessary – you may continue your usual activities (work, sport, etc.). After the scan, with or without injection, you can drive your own vehicle and return home normally. If a contrasting agent has been injected, you will be asked to drink a lot of water for the following 24 hours to accelerate its elimination. Should you feel any pain or abnormal sensation, please consult your GP or the department that conducted the scan.
And the results?
The images are analysed by a radiologist. A report of the obtained images is sent direct to the prescribing physician (and to your GP), who will explain them to you during a medical consultation; in certain cases, this report is given to you direct, along with the images. Keep them, file them and don’t forget to bring them with you at your next medical appointment.

